|
0 Comments
6000 BCE - Sharp bone and stone instruments are discovered in China, described as ‘pieces of stone used for treating illness by pricking the body’.
198 BCE - Burial tombs, amongst other artifacts unearthed in 1973, depict a medical practice related to acupuncture meridian systems. 552 AD - Acupuncture begins its migration from China to Japan and Korea. 1368-1600 - Acupuncture becomes one of the primary care systems used in China, alongside herbs, massage, diet, and moxibustion. 1500-1700 - The Dutch East India Company introduces acupuncture to Europe. 1822 - Acupuncture suffers a decline in China. 1880 - Acupuncture is introduced in Australia during the gold rush period by Chinese gold diggers. 1949 - Following the installation of the Communist government in China, all traditional forms of medicine are re-established and encouraged, including acupuncture. 1971 - In preparation for the unprecedented visit to China by US President Nixon, a US press corps member is treated with acupuncture following an emergency appendectomy. He describes his experience in the New York Times and as a result, teams of US physicians tour China to assess acupuncture's therapeutic applications. 1979 - The World Health Organisation conducts a symposium on acupuncture in China. 1997 - The National Institute of Health in the United States declares there is sufficient evidence of acupuncture's value to expand its use into conventional medicine. 2000 - Research into acupuncture as a medical treatment grows exponentially, increasing at twice the rate of research into conventional biomedicine. From 2000-2020, there have been over 13,000 studies conducted in 60 countries, including hundreds of meta-analyses. 2012 - Mandatory national registration of acupuncturists with the Chinese Medicine Board of Australia, under the governance of the Australian Health Practitioner Regulation Agency, a government body that manages the registration of all health practitioners. 2017 - The Acupuncture Evidence Project reviewed the effectiveness of acupuncture for 122 treatments over 14 clinical areas. Evidence of effect was found for 117 conditions, including knee osteoarthritis, lower back pain, and headache.
Thirty-eight other conditions had evidence of positive effect, including irritable bowel syndrome, menopausal hot flushes, neck pain, sciatica, and post-stroke rehabilitation.
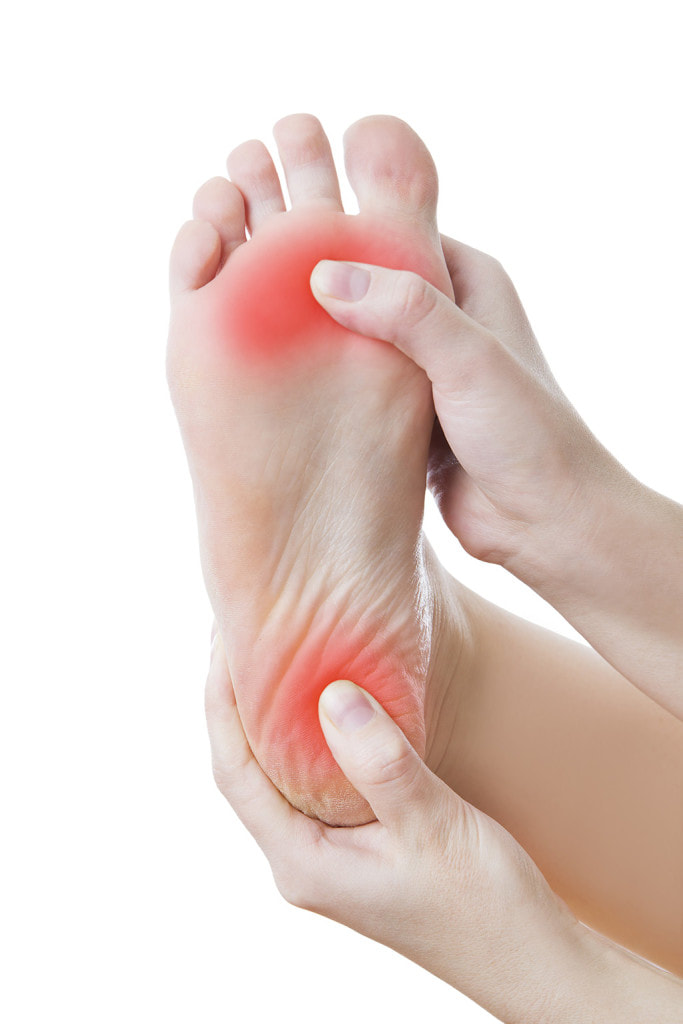
The symptoms often reported by our peripheral neuropathy clients include burning sensations, feeling of pins and needles, and numbness - particularly in the feet. Those with numbness often describe the feeling to be like wearing a thick pair of socks or walking on sponges. The symptoms alone however are usually not what prompts sufferers to come to our clinic for treatment; they’re typically more concerned about the impact neuropathy has on their quality of life, including:
|
Archives
May 2023
Categories
All
|







 RSS Feed
RSS Feed